The muddled COVID-19 strategy in the UK: herd immunity in all but name
In October 2016, the UK government conducted a national pandemic flu exercise, codenamed Exercise Cygnus. Ministers had to decide what to do as the overwhelming scale of the pandemic became apparent. In contrast to COVID-19, there was a treatment for, and vaccine against, this virus; yet the realities and outcomes were still sobering. The Civil Service report on the exercise and its “lessons identified” were not made public but the-then Chief Medical Officer told the World Innovation Summit for Health in December 2016 that the UK “could not cope with the excess bodies” and had “inadequate ventilation” in its hospitals.
Fast forward to 2020: the lack of testing is one of the key government failures. The World Health Organization early on declared testing as the key weapon against this virus. The National Health Service (NHS), which is already struggling with staff shortages, is now suffering under some of the highest staff absences it has ever seen because so many NHS staff are self-isolating fearing that they or someone in their family has the virus.

The inefficient and muddled way in which the UK government has handled the COVID-19 crisis has been shocking. The country had its first reported cases on January 31 and its first registered death on March 5. It took another seven days for the risk level to be raised from moderate to high.
The government at that point allowed the Cheltenham Festival to go ahead – an event which attracts more than a quarter of a million visitors. Partial school closures did not happen until March 18. Pubs, restaurants, clubs and gyms were not closed until March 20 – disastrously announced ahead of time, so many rushed to go out for a last pint. By this point, the UK had 3,983 confirmed cases and registered 177 deaths.
Procurement of equipment is another key government failure. The procurement fiasco has resulted in NHS workers having inadequate personal protective equipment. In this crisis, NHS doctors, nurses and other staff are dying as they try to save lives because they do not have the correct protective clothing, which is a scandalous failure.
Closer examination raises issues about NHS deployment, and its resilience to a pandemic crisis. It is plausible that the UK’s relatively high COVID-19 death rate is partly due to low levels of equipment and staffing. This can be seen by the following indicators, all per hundred thousand people: Hospital beds 2.7, doctors 2.6, intensive care beds 6.6. All much less than in other countries.
Given that the overall British levels of health spending are similar to many other countries, the issue appears to be on how the funds are distributed and spent within the NHS. These are fundamentally political decisions, taken by a series of Conservative governments and senior NHS management. These decisions have left the NHS in a more vulnerable position, making it less resilient than other health systems, and this is contributing to the higher observed death rates from COVID-19.
One of the main lessons for the government and NHS is that there has to be more spare capacity and higher levels of equipment to improve resilience to serious epidemics in the future. The UK did have pandemic disease at the top of the government risk register before coronavirus. But that was interpreted almost entirely as risk of a type of flu, rather than a SARS-type virus. In turn, that affected assumptions about speed of vaccine development and use of other drugs to slow transmission.
It is perhaps unfair to expect that the UK had previously stocked up on ventilators; there is an enormous risk of “fighting the last war”. But it has been comparatively short of intensive care units while an ageing population and tight budgets have strained its capacity. Like in Spain and in Italy, 10 years of austerity will cost lives.
Boris Johnson’s government and his senior health advisers were complacent and ill-informed when they advocated the “herd immunity” approach which was explained by the Chief Scientific adviser Sir Patrick Vallance officer on BBC Radio 4 on 13 March 2020. The British government and its official scientists did not spot what was so evident elsewhere. They had the chance to learn from what was happening in China, Italy and Spain. It was an astonishing failure of leadership and of good governance. But Chris Whitty, the UK’s chief medical officer, and Patrick Vallance share the blame. Did they get their advice wrong, or did they fail to speak truth to power and to the public? While the NHS is being overwhelmed with critically ill patients, the government has looked out of its depth and vacuous.
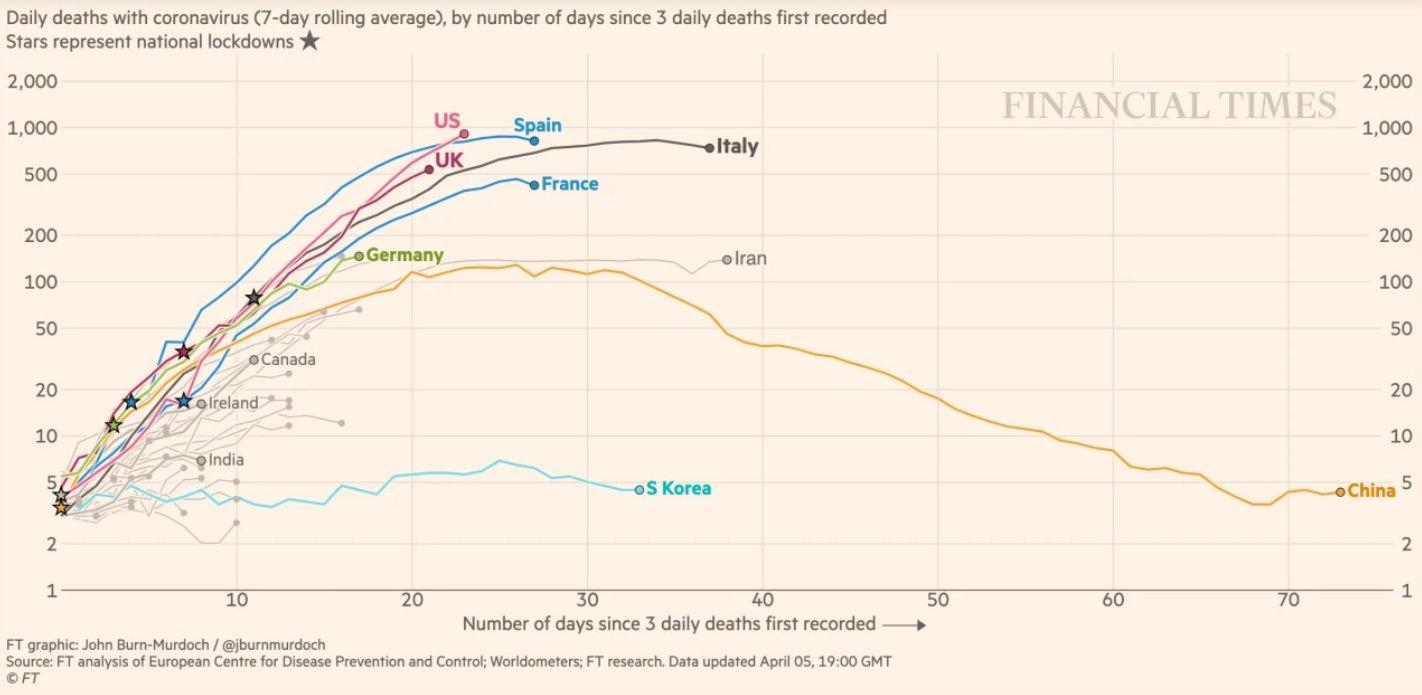
The government’s most recent pledge to increase virus testing to 100,000 a day for England by the end of April is a late response to the problems but also difficult to achieve. Home Secretary Priti Patel needs to explain why many flights arriving from China, New York, Spain and Italy have not been checked for the health of the passengers. The UK could pass Spain for peak daily deaths and possibly Italy.
Whether clueless or reckless, the slowness in response leads to the conclusion that government policy in all but name still seems to be the herd immunity approach. The herd immunity policy is inhumane, deeply flawed and unethical. The Johnson government must be held accountable for these initial decisions.
